
May 9, 2024
DICOM
Education
Navigating the Evolution of Image Exchange in Healthcare
Welcome to our exploration of Image Exchange in healthcare, a cornerstone of modern medical practice. As healthcare continues to evolve, the seamless transfer of medical images across various facilities has become crucial for delivering high-quality care.
Introduction to PACS and Transition from Physical Films
Before the adoption of Picture Archiving and Communication Systems (PACS), distributing medical images typically involved physical films, which were cumbersome and limited in accessibility. The introduction of PACS marked a substantial advancement, signaling the beginning of the digital imaging era initially facilitated by CDs and DVDs. This shift from physical film to digital media represented a tremendous leap forward in how medical images were stored and shared.
However, this transition also introduced complex challenges related to integrating these digital media into local PACS. Although moving to digital was a step forward, the integration process required considerable human effort and meticulous attention to detail. For an external or foreign study to be successfully reconciled within a local PACS, for many PACS, it is essential to generate an HL7 ORM message and thoroughly localize all details of the outside study to align with the specific requirements of the importing PACS. If this localization process is not performed correctly, the imported study can end up in an exception worklist.
Many PACS systems require each study to be associated with an HL7 ORM message, and in the absence of this association, the study may be tagged as RIS unverified/unspecified. Furthermore, even in systems that are not ORM-dependent, accurate localization remains crucial. If the foreign Patient ID is not correctly mapped to mirror the local Patient ID, the imported record will not file within the patient's existing jacket. This misfiling can disrupt clinical workflows and delay patient care.
The process of integrating a single study from CDs or DVDs into PACS can take between 10 to 30 minutes, highlighting the ongoing challenges and the significant labor involved in ensuring seamless data compatibility and integrity across different systems. This phase of integration emphasizes the necessity for continuous improvements in the way medical images are handled and integrated into healthcare IT systems to ensure efficient and effective patient care.
Over the years, the use of CDs and DVDs has declined, influenced by initiatives like the ACR's #DitchtheDisk and the broader shift away from these formats in consumer electronics. This trend has accelerated the adoption of fully digital solutions, which enhance accessibility and reduce the operational burdens of physical media.
Digital Alternatives and Their Integration
While physical media like CDs and DVDs continue to be used, the increasing adoption of image-sharing networks and regional Health Information Exchanges (HIEs) has significantly reduced their prevalence in healthcare. These digital alternatives offer a more efficient means of exchanging medical images and reports, significantly reducing the reliance on physical media. Despite the shift away from physical media, the critical need to reconcile an outside study to be compatible with local Picture Archiving and Communication Systems (PACS) remains unchanged. All the requirements for localizing a study and creating an HL7 ORM message, reminiscent of the CD era, are still essential in these digital workflows.
Moreover, many sharing networks and HIEs now incorporate Vendor Neutral Archives (VNAs) and DICOM brokers, which support the automation of ORM generation, Patient ID localization, and terminology management, enhancing the integration process and maintaining the integrity of medical data within PACS. In cases where automated reconciliation tools are not available, the time required to import a study from a digital sharing solution is expected to remain approximately the same as during the CD era, typically ranging from 10 to 30 minutes. This emphasizes the importance of continued advancements and the adoption of automation in healthcare information systems to improve efficiency and accuracy in medical imaging management.
Handling Terminology and Procedure Codes
The management of medical terminology is a crucial aspect of image exchange processes. Many Picture Archiving and Communication Systems (PACS) may react adversely if an imported study contains a procedure code and description that do not match the predefined list of procedures recognized by the PACS. This discrepancy can lead to integration issues and disrupt clinical workflows. Additionally, the absence of a standardized terminology dictionary complicates the pre-fetching of relevant exams, which is essential for efficient healthcare delivery.
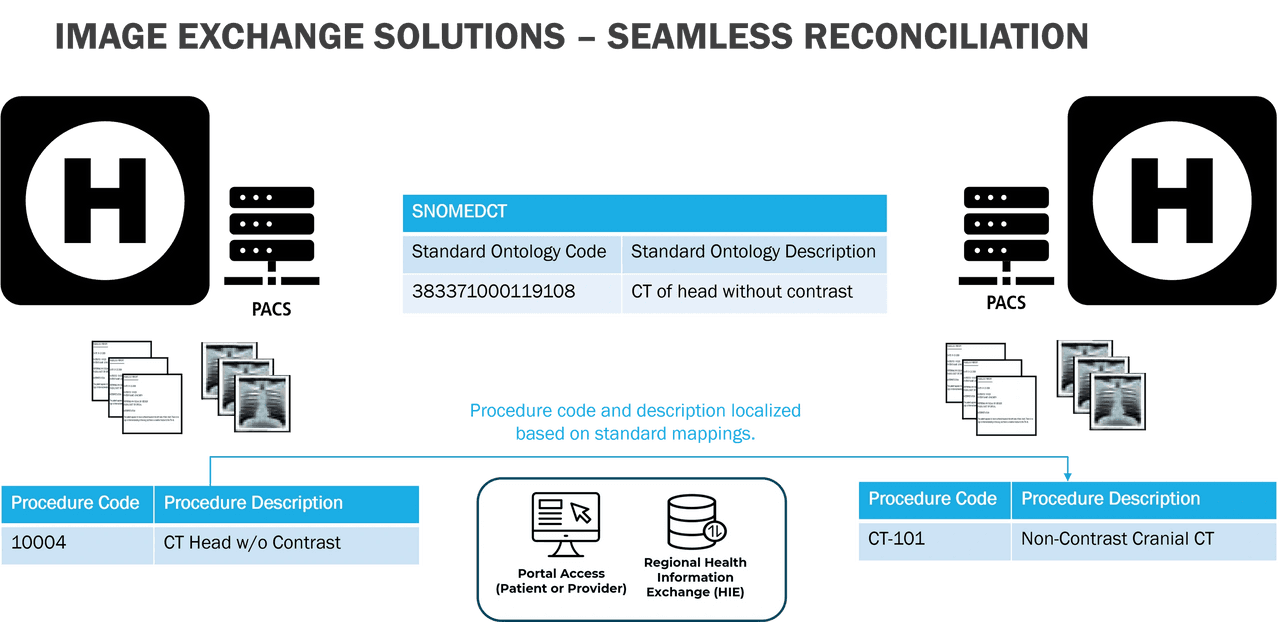
To address these challenges, terminology reconciliation is typically handled manually. This involves healthcare professionals performing a detailed mapping exercise, where local procedure codes at each site are aligned with a standard ontology. The goal is to ensure that all exams across a network or Health Information Exchange (HIE) are mapped to a regional ontology, thereby building out semantic interoperability.
These mapping rules often support a many-to-one relationship, where multiple local procedures may correspond to a single ontology code. While this system promotes consistency across different healthcare settings, the initial mapping and ongoing maintenance are time-consuming and resource intensive. Additionally, if a healthcare facility updates its Hospital Information System (HIS) or Electronic Medical Record (EMR) system, all newly introduced procedures must be manually re-mapped, further adding to the complexity and workload.

The manual nature of this task emphasizes the need for advanced solutions, possibly incorporating automated mapping technologies, to enhance efficiency and reduce the burden on healthcare providers.
Streamlining Medical Terminology Management: Time Savings with AI and ML
The integration of Artificial Intelligence (AI) and Machine Learning (ML) into medical terminology management, as discussed in the 2019 paper "Sharing is Caring: Exploring machine learning-enabled methods for regional medical imaging exchange using procedure metadata," has significantly transformed the workload for healthcare administrators and mappers. These technologies automate the mapping of local procedure codes to standard terminologies such as SNOMED CT, achieving efficiencies with accuracies up to 96.3%. This automation reduces the extensive manual effort previously required, substantially freeing up time for administrators who were once tasked with these complex and repetitive mapping processes.
With the adoption of AI-driven systems by Imaging vendors, the need for human intervention in the mapping process has dramatically decreased. This has led to faster updates and adjustments to terminologies in real-time, which is essential for keeping pace with the rapid changes in medical practices. Consequently, administrators and mappers can now focus more on strategic tasks and improving healthcare delivery rather than getting bogged down by the intricacies of manual data management.
This shift not only represents a significant step forward in making medical data management more efficient but also enhances the scalability and reliability of healthcare systems. By automating tedious tasks, AI and ML technologies are ensuring that healthcare databases remain accurate and up to date without the continuous need for manual oversight, thereby providing substantial time savings and reducing the potential for human error.
Other Considerations
Accession Number Localization
When a foreign exam is ingested into the local PACS, it often necessitates some form of modification to the accession number to prevent conflicts with local studies. A common practice is to append or prepend a suffix or prefix to the accession number, which might include a mnemonic or acronym derived from the "ISSUER_OF_PATIENTID" (DICOM tag 0010,0021), indicating the originating organization of the study. This approach helps in identifying the origin of the study while ensuring that the modified accession number does not exceed the maximum character limit supported by DICOM for accession numbers, which is 16 characters. Ensuring these modifications are handled correctly is crucial to prevent any negative impacts that could arise from accession number conflicts.
Data Retention Policies
Another critical aspect to consider is the policy regarding the retention of ingested exams. Different organizations may have varying policies based on local governance frameworks. Some may choose to retain all ingested exams indefinitely, never purging imported data, to ensure a comprehensive historical record is maintained. On the other hand, some organizations opt to regularly purge older exams. This approach guarantees that the most recent copies of exams are retrieved from the network or Health Information Exchange (HIE), minimizing the risk of retaining outdated or altered exam data in the local PACS. Decisions on data retention should align with organizational policies and the overarching goal of maintaining accurate and current medical records.
Conclusion: Transforming Healthcare Through Advanced Image Exchange Technologies
As we conclude our exploration of the evolution of image exchange in healthcare, the transition from physical media to advanced digital solutions like PACS and HIEs marks a significant advancement in the field. This transformation has not only simplified the storage and sharing of medical images but also introduced complexities that require innovative solutions and continuous improvement.
The shift from CDs and DVDs to digital image-sharing networks and regional Health Information Exchanges has reduced the reliance on physical media, enhancing the accessibility and efficiency of medical image exchanges. Despite these advancements, the need for meticulous integration processes like HL7 ORM message generation and patient data localization remains, underscoring the importance of ongoing technological enhancements.
The manual tasks associated with mapping and managing medical terminologies in PACS, which often become bottlenecks in clinical workflows, are being transformed by AI and ML. These technologies automate critical processes, reducing the workload for healthcare administrators and mappers significantly. This automation not only speeds up the process but also improves the accuracy and reliability of medical data across healthcare systems.
As healthcare continues to evolve, the integration of these advanced technologies within healthcare IT systems will play a crucial role in ensuring efficient, reliable, and scalable medical image and data management. By continuing to embrace and refine these digital solutions, the healthcare industry can look forward to enhanced interoperability and streamlined workflows that ultimately improve patient care and outcomes.
Want to Keep Learning?
To deepen your understanding and further explore the intricacies of imaging informatics, consider diving into our course "IMG_101: Introduction to Imaging Informatics," designed to expand your knowledge of imaging informatics and prepare you for the CIIP exam. Visit our learning platform for more information






